Key takeaways
- Manual scheduling can’t scale fairly. Complexity across specialties, sites, and regions requires rule-based automation.
- Equitable scheduling depends on consistent application of clear rules. Automation ensures fairness isn’t subjective.
- Transparency builds trust. When physicians see how shifts are distributed and why, equity becomes visible and sustainable.
Physician burnout doesn’t start in the exam room.
More often, it starts in the schedule.
When night shifts, weekends, holidays, and high-intensity shift placements are unevenly distributed, dissatisfaction grows quickly. What starts as frustration turns into disengagement. Over time, inequitable scheduling contributes to turnover, recruitment challenges, and strained team dynamics. Or, at the very least, tension-filled teams.
The issue isn’t effort. Most physician leaders and administrators work hard to create fair schedules. Yet, 75% of physicians in Canada say their administration workload is an impediment to caring for patients.
The real challenge isn’t defining fairness, it’s building the infrastructure that makes equitable scheduling transparent, simple, and able to scale.
Ease of implementation and change management
That infrastructure must also support adoption. It should minimize change management friction, integrate seamlessly with existing systems, and require minimal ongoing training. Teams and situations change in dynamic healthcare environments. The tools around you need to adapt with teams and departments, not stuck in neutral. When workforce management tools are intuitive and interoperable, equity becomes easier to sustain and remain consistent.
Traditional group-level scheduling systems, too often powered by closed spreadsheets, legacy tools, paper print outs scattered around, or even Post-it notes, were never designed to manage today’s complexity. They struggle to account for specialty-specific rules, multiple sites, regional coverage needs, varying FTE levels, and evolving absence patterns.
Equity in scheduling doesn’t happen by chance. It requires intentional design that’s repeatable and scalable through the right workforce management foundation.
Clinicians save an average of 161 hours annually using Petal Billing.
The equity gap in physician scheduling
On paper, most schedules appear balanced. Everyone has roughly the same number of shifts.
But true equity goes deeper than simple counts.
It considers:
- Weighted distribution of nights, weekends, and holidays
- Specialty qualifications and coverage requirements
- Experience levels and supervision needs
- Part-time and variable FTE structures
- Multi-site rotation balance
- Protected time and leave policies
Without a structured system, these variables are handled manually that increases the risk of inconsistency, bias (intentional or not), and fatigue-driven decision-making.
As physician groups grow across departments and regions, the complexity compounds. What once worked for a 25-provider group breaks down at 150 providers across multiple departments and sites.
As teams scale, equity becomes harder to maintain.
3 Steps to build equity into physician scheduling
Step 1: Establish clear, weighted fairness rules
Equity starts with definition and the agreed upon terms that make up the rules needed to be followed.
Leadership teams must determine:
- How are high-burden shifts weighted?
- How should nights and weekends be distributed?
- How do specialty constraints influence eligibility?
- How are new hires onboarded into rotations?
- How are multi-site assignments balanced?
- How are absences and leaves factored in?
Without clearly defined rules, fairness becomes interpretive. And interpretation leads to inconsistency.
Documented, agreed-upon rules create the foundation for equity. But they must also be operationalized. There’s no point in creating clearly defined rules and definitions if there are going to sit on a virtual shelf collecting dust.
That’s where automation becomes essential.
Step 2: Automate scheduling with a fairness-driven engine
Spreadsheets can’t consistently apply complex, weighted rules across dozens, or hundreds of providers.
An automated scheduling engine built for physician workforce management allows teams to:
- Apply fairness rules uniformly to every provider
- Balance high-burden shifts automatically
- Respect specialty and qualification requirements
- Integrate absence tracking and availability
- Scale seamlessly across departments, sites, and regions
- Reduce manual administrative hours
Automation removes subjectivity.
Instead of relying on memory or negotiation, the system enforces predefined rules. Every provider is scheduled using the same logic.
Equity becomes embedded into the structure, independent of who is building the schedule that month. Not to mention the speed those schedules are built creates more time that will be put back into care, or at the very least not stuck working on a spreadsheet.
As organizations grow, this consistency becomes critical. Manual processes break under scale. Automated systems adapt.
Did you know Petal customers have seen a 98% reduction in manual scheduling work?
Step 3: Build transparency into the scheduling experience
Even a fair schedule can feel unfair if the logic behind it is invisible. Transparency is the multiplier that turns automation into trust.
Modern workforce management systems should provide:
- Clear visibility into shift distribution metrics
- Individual workload summaries and real-time tracking for fast decision making
- Self-serve shift swaps within defined rules
- Calendar synchronization for clarity and planning
- Data dashboards showing equitable allocation over time
Where physicians see:
- How many nights or weekends they’ve worked and on call
- How that compares to their peers
- Why certain assignments were generated
- How swaps are approved and tracked
Transparency transforms scheduling from a black box into a shared system.
Self-serve tools also empower physicians to manage their schedules collaboratively. Shift swaps can occur within rule-based guardrails, maintaining fairness while increasing autonomy. Absences are tracked consistently. Calendar sync reduces miscommunication.
Instead of sending emails or relying on informal arrangements, the process becomes structured and visible.
Transparency reduces friction. It builds accountability. And it reinforces equity over time.
Why scheduling equity is a strategic imperative
Healthcare organizations are facing mounting workforce pressures:
- Burnout and retention challenges
- Expanding multi-site operations
- Increasing regulatory and compliance demands
- Growing physician expectations for flexibility
Equitable scheduling directly impacts all of these areas.
When physicians trust the scheduling process, teams function more cohesively. When administrators spend less time resolving disputes, they can focus on strategic workforce planning. When shift distribution is balanced across sites and specialties, organizations scale more effectively.
Equity isn’t just an operational concern; it’s a cultural one.
A system that consistently applies rules, scales across departments and regions, and makes fairness visible sends a powerful message: every provider is valued fairly.
The future of physician workforce management
The next generation of physician scheduling is defined by four pillars:
- Automation that applies fairness rules consistently
- Scalability across departments, sites, and regions
- Transparency that builds trust and accountability
- Change management that adapts quickly to maintain coverage
Workforce management systems must go beyond static schedule creation. They must support dynamic environments where absences, swaps, and expansion are constant realities, and clinicians and administrators alike have the tools at hand to do that.
Create equity by design
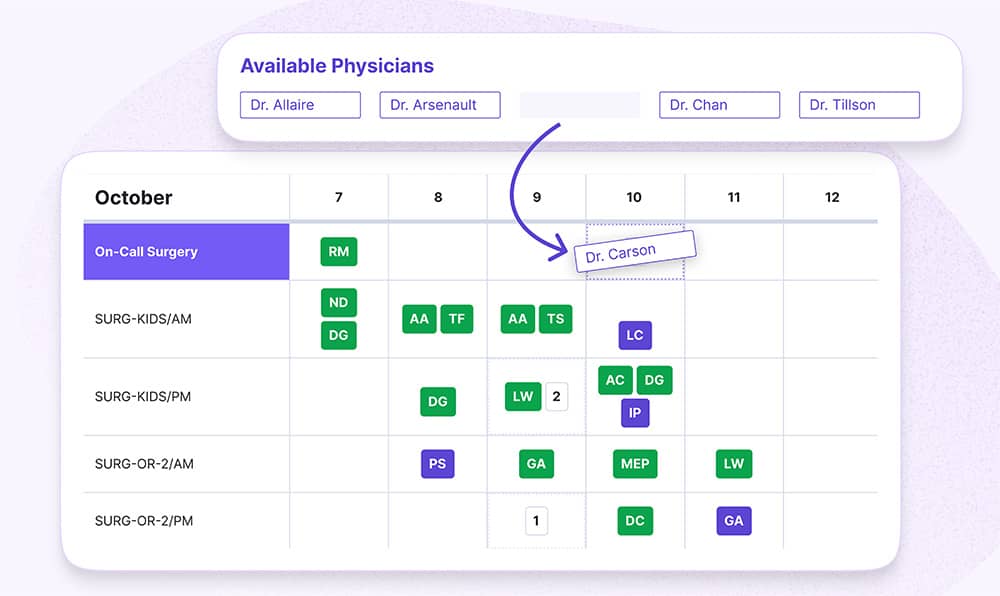
If your organization is still relying on manual scheduling tools that struggle to handle specialty rules, multi-site coverage, or equitable shift distribution, it may be time to rethink your approach.
A purpose-built physician workforce management solution can help you:
- Automate scheduling equitably and efficiently
- Scale across departments and regions
- Enable self-serve shift swaps and centralized absence tracking
- Synchronize calendars seamlessly
- Make fairness visible through transparent reporting
Ready to build equitable, scalable scheduling systems that strengthen physician teams?
👉 Explore Petal Workforce Management.
Because equitable patient care starts with equitable physician schedules.







