Points clés à retenir
- Overburdened emergency departments feed a negative care loop. Patients, providers, and decision-makers all struggle to achieve satisfying outcomes.
- Value-based care realigns system-wide priorities. Structural focus turns to measurable outcomes rather than metrics like number of visits.
- Real-time care orchestration provides a path forward. Rerouting patients away from EDs to more appropriate care settings meets every health system stakeholders’ needs.
Timely access to care is critical to Canada’s health system sustainability.
Yet, patients across the country often turn to emergency departments (EDs) for non-urgent care because they lack primary care options or don’t know where else to go. The result? Overcrowded EDs, surging system costs, and a demoralizing experience for all involved. This feeds a crisis loop of declining care quality.
In Ontario, the Auditor General reported that some hospitals saw up to 14% of patients exit without care in 2023.
Read on to learn how value-based care rethinks health systems’ supply demand matching to benefit patients, providers, and decision makers.
System-wide healthcare challenges demand action
Overburdened EDs paired with inadequate primary care options causes enormous strain on Canada’s health system.
In practice, this means patients are increasingly walking into EDs and leaving before receiving care. The portion of patients leaving without being seen increased in most provinces from 2019–24. Prince Edward Island, New Brunswick, and Manitoba saw double-digit exit rates with PEI peaking at roughly 1 in 7 patients giving up on their ED care.
- Why patients leave: Long wait times of 5.5 hours per visit nationally cause patients to wait at home, self-treat, or seek alternative care options.
Concurrently, Canada’s primary care access ranks below most global peers. This leads many patients to seek emergency care when clinics or pharmacies would more effectively address their issues. A recent Canadian Medical Association survey found that 5.9 million adults in Canada lack primary care options.
For clinicians in Canada, administrative burden costs nearly 20 million hours annually. That’s time away from caring for patients—the core pursuit of most clinicians entering the field. This leads to frustrated patients and providers. Clinicians and their team would improve the country’s ED and primary care challenges if they had greater capacity to treat more patients faster.
Instead, we see compounding impacts of the negative feedback loop:
- More overcrowded emergency rooms.
- Increased burnout among frontline staff.
- Worse patient care outcomes.
Without action, the healthcare system will continue driving overworked healthcare professionals out of the field. Patients will wait even longer in EDs (if they wait at all), more EDs will close, and system strain will increase further.
The Quebec government redirects 800+ patients daily to more appropriate care.
Value-based care breaks the healthcare crisis loop
Value-based care garners its “value” from targeting each stakeholders’ unique needs within the care loop. It measures care by outcomes rather than metrics like number of visits.
One way to achieve this: orchestrated care in real-time.
This is achieved by restructuring patient routing to ensure patients receive care at the most appropriate care setting. For example, a patient with an earache likely doesn’t need ED care—but without a primary care option, they may feel the ED is their only option. These low-acuity (CTAS 4–5) ED visits leave individuals with higher-acuity needs waiting.
Real-time orchestration guides value-based care by emphasizing prevention, coordination, and efficiency. Considering each stakeholder:
- Patients gain access to faster, more effective care in pharmacies and clinics rather than waiting in EDs.
- Providers decrease their workload through alleviated ED burden, allowing them to treat patients who most need their support.
- Decision-makers gain economic benefits from better-treated patients and more efficiently utilized healthcare resources.
To make this work, primary care visits must be made visible and bookable; systems must be connected, including linked EMRs, booking portals, and referral lists, so capacity is visible; clinicians must be freed from paperwork, such as through automated scheduling and billing solutions, to return time to patient care.
The impact is immediate when every part of system-wide care is aligned. Action now will create compounding benefits for generations to come.
CHUM achieved 92% clinician satisfaction with the Petal Workforce Hub.
Petal Patient Hub: Right care, right time
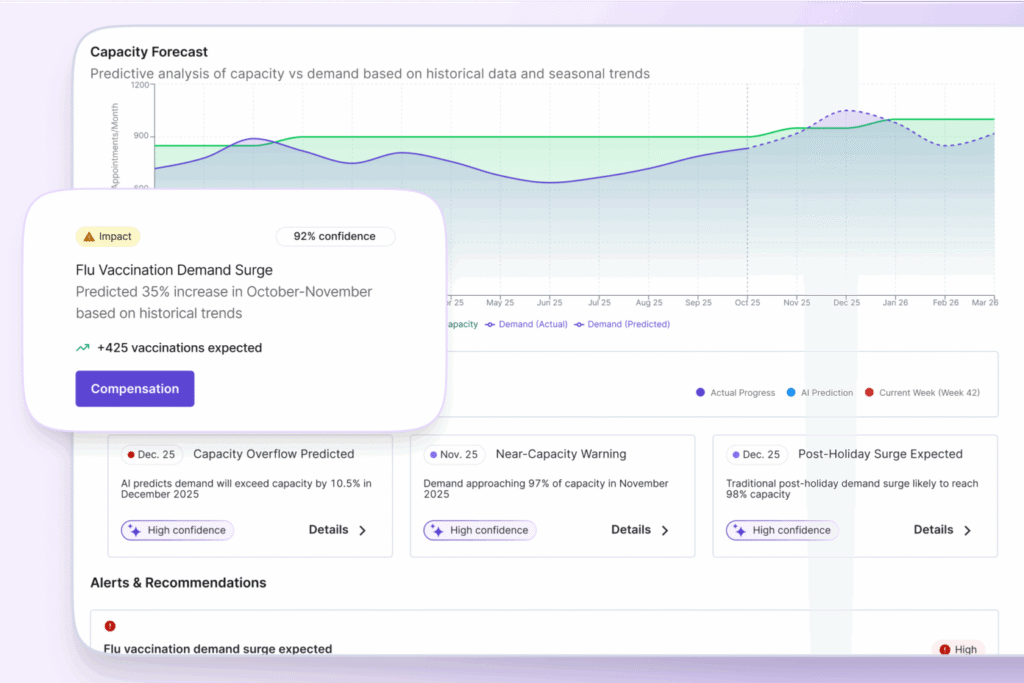
Advanced solutions address inequitable care access while generating millions of dollars in economic benefits.
The Hub Patient centralizes patient care requests at every entry point. It routes patients to the right care in real time and gives health leaders full visibility into capacity across the health system.
Independent proof: In Quebec, the Patient Hub connects 850 clinics and 19,000 professionals in one network. This led to:
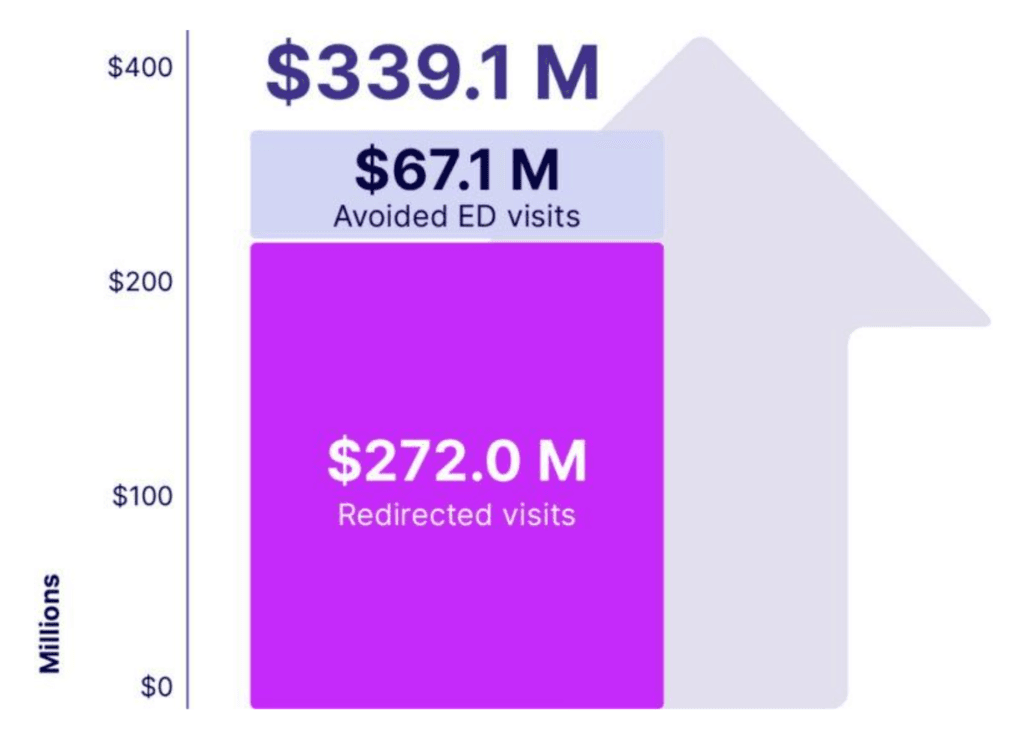
- $339M in cumulative economic value since 2022; $121M annually in 2024–2025—$2.3M per week.
- 814,000 ED visits avoided and 353,000 redirected to primary care.
- 12.5% fewer low-acuity ED visits (CTAS 4–5) compared to pre-Hub levels.
Moreover, 811 health services provide a critical access point. In 2024–2025, 23% of calls resulted in booked primary care visits—up from 15% in 2022–2023. That’s 710 calls per day routed to more appropriate care settings.
Scalable, coordinated care is possible and sustainable. Let’s make it work together.
Reduce ED overcrowding for patients and your staff:







