Key takeaways
- Analytics enable proactive care: Healthcare leaders anticipate demand and act earlier, positioning their organizations for sustainable growth.
- The advantages are proven: Improved patient flow, capacity management, and provider wellbeing follow smarter budget allocation.
- Value comes from operationalization: Analytics compliment strategic approaches to structuring care resourcefully where insights embed into existing workflows.
Healthcare systems need modern solutions to modern problems.
Hospitals and other care facilities face persistent staffing shortages and overcrowded emergency departments (EDs), as strained budgets make addressing these issues more difficult. Patient demand only continues to increase. In Canada, 5.9 million adults lack access to primary care while 79% of the health workforce reports feeling burnt-out.
In response, healthcare organizations turn to advanced solutions. Among them: data analytics.
When providers predict where patient demand will be in the future, whether it be one hour or one week, they make better decisions for their patients and teams.
- What are analytics? Insights derived from historical and real-time data, combined with statistical models and machine learning, to forecast what is likely to happen next.
Beyond understanding what might happen, healthcare organizations increasingly deploy these insights throughout their care systems. Read on to explore how analytics make healthcare teams work smarter and faster for more people.
Why healthcare systems need data analytics
The challenges facing healthcare systems are both structural and immediate.
Many care settings are overcapacity. This frustrates patients and worsens care outcomes. It makes staff burnt-out: 49% of family physicians in Canada reported working beyond their desired capacity; 90% of nurses report some level of burnout; and more than 50% of physicians plan to cut their hours.
Fundamentally, many healthcare organizations struggle to match supply with demand.
Available care providers, whether in hospitals, clinics, or pharmacies, may have space available to patients. Patients with issues ranging in acuity who desire professional support could be effectively treated in one of these spaces. But too often, EDs are the focal point for treatment and frontline staff become overworked.
Long ED wait times—5.5 hours per visit nationally between 2024–25—lead patients to exit EDs to wait, self-treat, or seek alternative care. Care teams are forced into constant triage mode. Schedules are frequently adjusted at the last minute. Inefficiency reigns.
Alongside ED burden, further challenges include:
- Lengths of patient stay
- No-show appointments
- Rising overtime hours
This is where analytics make a meaningful difference.
The Quebec government redirects 800+ patients daily to more appropriate care.
How healthcare teams use analytics
The value of analytics is most tangible when applied directly to operational workflows.
For example, instead of reacting to overcrowded EDs, teams use patient flow management to anticipate surges in demand and adjust staffing or redirect patients accordingly. In practice, it’s critical that patients and providers have somewhere—such as clinics or pharmacies—to flow patients toward when they exit EDs. This kind of real-time orchestration helps reduce overcrowding while improving the quality of care.
- Complimentary advantages: Redirection is a use case highlighting how analytical insights are one piece of larger strategic approaches in seeking intelligent, network-wide growth.
Capacity planning is another critical application. Predictive models forecast peak periods across departments, such as in EDs or outpatient clinics, allowing organizations to plan staffing levels and adjust schedules accordingly. Rather than relying on static schedules or historical averages, teams dynamically align capacity with expected demand.
To visualize analytical insights, real-time dashboards connected to health systems show what’s happening where. These forward-looking views enable more informed decision-making without requiring a PhD in Statistics.
These capabilities are measurably beneficial.
Proving impact in Canada: Petal’s Patient Hub helped a provincial health authority avoid 814,000 ED visits and redirect 353,000 patients to primary care by forecasting demand.
Predicting discharges and flow: A machine learning model estimated short-term discharges, long-stay patients, discharge destination, and ICU flows in the 80%+ accuracy range. This study used a major hospital’s existing EHR data.
Reducing staffing costs: Hourly ED staffing costs were reduced by over $160 without negatively affecting throughput using a prediction-driven staffing framework.
These results display how analytics-supported care coordination saves teams time and money. Rather than operating in silos, departments align around a shared understanding of future demand. This leads to a better match between supply and demand across the entire system.
When resources are distributed more effectively, staff experience less friction and stress in their daily work. Patients win when their providers have more time and energy for care.
Sourcing data makes analytics possible
Analytics offer healthcare organizations a way to move from reactive problem-solving to proactive design.
Analyzing patterns in historical and real-time data allows predictive models to forecast patient volumes, identify bottlenecks, and anticipate resource needs before issues arise. This allows healthcare teams to structurally pivot from reactivity to proactivity.
Data is key to making analytics work, and electronic medical record (EHR) adoption is a vital source of data. Adoptions rates in the United States reached 96% of non-federal acute care hospitals in 2022 (up from 28% in 2011). Canadian care settings lag this figure but hold tremendous opportunity to effectively deploy cross-facility tools due to Canadian healthcare being structured at the system-level.
Operationally, analytics enable efficient resource management. Staff are aligned more closely with actual demand, allowing more predictable workloads and fewer last-minute disruptions. Rooms and equipment are utilized more effectively. Bottlenecks are identified, and then mitigated, before they disrupt care. Patients experience shorter wait times. Organizations reduce waste—both in time and cost—by moving resources to where they’re needed.
The result is a smoother, more coordinated system.
Clinicians save 3.1 hours per week an average using Petal Billing.
Forecast your network capacity in real-time
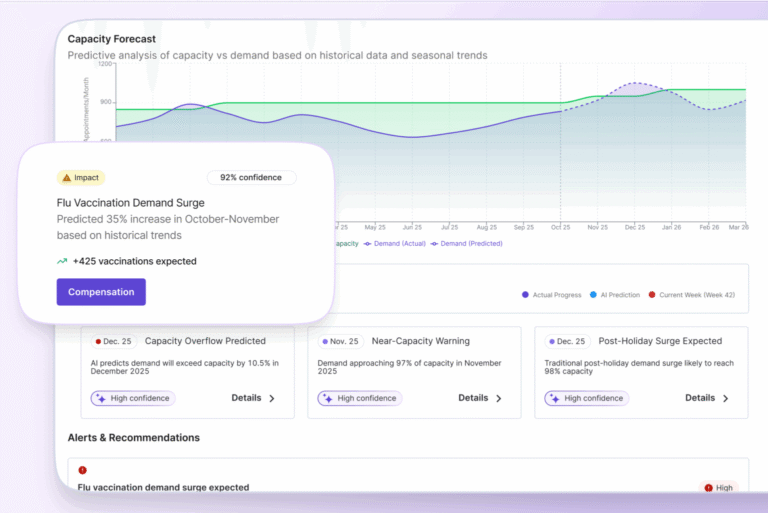
Advanced solutions need providers who are ready to advance.
Petal’s Patient Hub helps forward-looking teams deliver better care, faster. Along with the redirection advantages described above, Quebec reduced low-acuity ED visits by 12.5% and gained $339M in economic benefits using the Patient Hub.
Innovative features make the Patient Hub possible:
- Centralized care requests to capture patient preferences and history
- Integration with EMRs, PMS, and online booking portals
- Predicted demand to drive high impact resource allocation.
Let’s make your network future-ready through the power of analytics.
Reduce ED overcrowding for patients and your staff:






