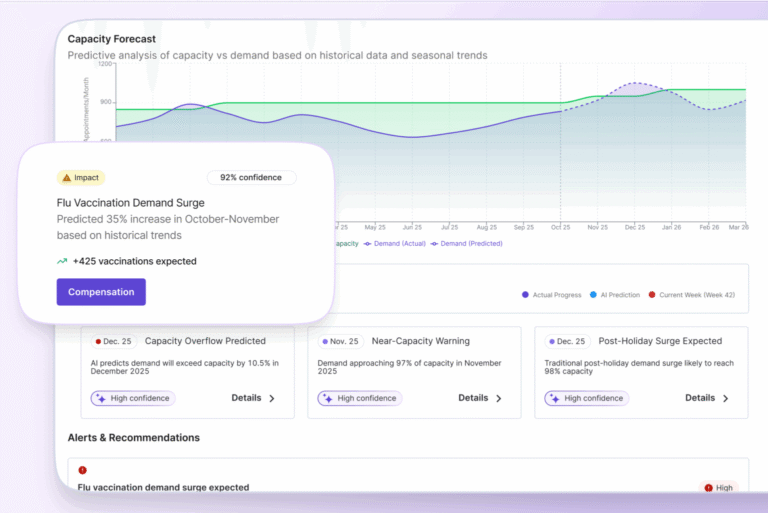
Key takeaways
- Pharmacies unlock untapped system capacity: Redirecting low-acuity patients away from EDs to pharmacies ensures healthcare resources are used where they’re needed most.
- Easing ED pressure breaks the burnout cycle: Fewer unnecessary visits mean more manageable workloads, leading to better work-life balance.
- The financial impact is measurably great: Redirecting patients generates system-wide savings for reinvesting into improved patient access and provider wellbeing.
Pharmacies help reduce emergency department overcrowding by redirecting low-acuity patients to more appropriate care settings, faster. This improves wait times, reduces provider burnout, and lowers system costs.
Overworked providers and strained healthcare budgets need relief. That’s where pharmacies come in.
Maximizing system resources is imperative for Canadian health systems. Currently, many patients seek treatment in emergency departments (EDs) because they lack primary care options. Long ED wait times—5.5 hours per visit nationally between 2024–25—frustrate patients and exhaust providers. This is compounded by 14% of ED visits being manageable by primary care; 50% are addressable by virtual care, such as 811 systems.
Patient redirection offers an advanced solution for moving patients to the right care, faster. Pharmacies are critical nodes in this network. When ED providers direct patients to the most appropriate care in real time, wait times decrease and patient lives improve.
Here are three ways pharmacies unlock capacity to ease strain on patients and providers while stretching budgets.
How do pharmacies reduce ED overcrowding?
Pharmacies absorb low-acuity cases that don’t require hospital resources. When patients are redirected in real time, EDs save space to prioritize higher-acuity care.
System wide, something has to give: 5.9 million adults in Canada lack access to primary care and 79% of the health workforce reports feeling burnt-out.
Let’s explore the impact on ED capacity.
A patient goes to an ED with a low acuity case, such as an ear infection or a rash, that could be addressed in a clinic or pharmacy. They’re now in line within the ED. After them, a patient arrives with a higher acuity case, such as severe abdominal pain, that must be solved in the ED that day. As both cases are non-life threatening, the second patient may wait longer than they should because the first patient is already waiting.
Now, let’s imagine the hospital is part of a network that redirects patients to local clinics and pharmacies.
When the patient with the ear infection arrives, the hospital identifies a local pharmacy with space. The patient is redirected to this pharmacy rather than taking up space in the ED. This saves ED capacity, so when the second patient arrives, they’ll see a provider faster.
- Remember: The fundamental goal is to match supply with demand more efficiently.
Better outcomes begin by connecting patients to care providers within the larger health system in real time.
In summary: Patients, providers, and health authorities are on the same team. When the network effectively connects patients with care, everyone wins. The challenge is typically coordination and visibility.
Quebec achieved 12.5% fewer low-acuity ED visits (CTAS 4–5) compared to pre-Patient Hub levels.
Why does redirecting patients reduce ED burnout?
When EDs are overcrowded with non-urgent cases, providers face constant time pressure and longer shifts. This environment increases cognitive load, straining providers and limiting attention for patients.
By diverting appropriate patients to pharmacies, care teams can spend more time per critical case, while reducing overtime and stabilizing workloads.
Today, healthcare professionals in EDs are especially susceptible to burnout due to the intense demands of their roles.
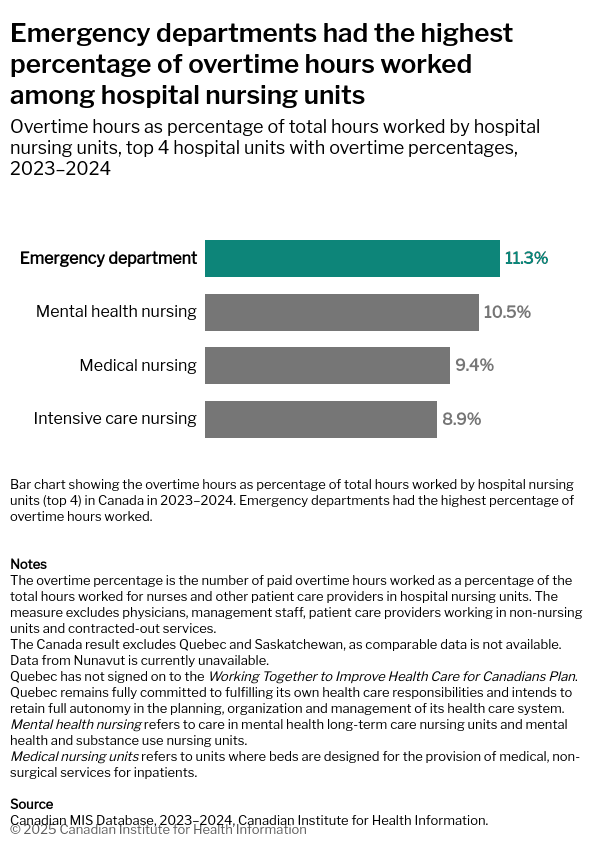
The scarcity of physicians and other essential healthcare professionals combined with strained budgets and mounting ED pressures place immense strain on providers, as well as Canada’s public health systems. For example, as the above graph shows, ED nurses face longer days than nurses in any other field.
- In 2024, one out of every five hospitals with an ED or urgent care centre had unplanned shutdowns.
This drives a negative feedback loop of overcrowded EDs driving clinician burnout, leading to higher turnover rates, which leaves fewer clinicians to support patients, causing longer wait times and even more crowded EDs.
But when pharmacies reduce ED overcrowding, the pressure on frontline providers eases.
Patient redirection can use pharmacies to break the cycle of strain that causes mismatched supply and demand. This means ED teams see fewer patients while spending more time with the patients they do see.
Overtime hours decrease and work-life balance improves. This increases retention rates, saving critical funds that would otherwise be spent recruiting, hiring, and training new staff members. These costs are then redistributed to other areas within the care system, making a more prosperous healthcare experience for patients and providers.
When pharmacies are an outlet for low-acuity ED cases, pharmacists enjoy greater impact and ED teams achieve much-needed balance. And pharmacists see the potential for more traffic to their thriving pharmacy.
In summary: Pharmacies offer a vital off-ramp for low-acuity cases that would otherwise stretch already burnt-out ED teams, helping support a stronger healthcare continuum and pharmacies as well.
$339 million in cumulative savings since 2022 in Quebec? That’s Patient Hub.
What are the financial benefits of patient redirection?
EDs are one of the most expensive points of care. So, when patients with minor conditions are treated in pharmacies or clinics instead, systems reduce unnecessary resource use, shorten hospital stays, and lower admin burden.
Patient redirection pays for itself through enormous, system-wide economic benefits, which are then reinvested into improving access and capacity.
As proven by Quebec’s patient redirection implementation, these include:
- Enhanced ED efficiency: Reduced administrative costs and shorter waiting times, as well as reduced risks of infection, through smarter ED management.
- Better access to primary care: Fewer hospitalizations and shorter length of hospital stays by connecting patients with faster care via primary care partners.
- Higher productivity: Reduced work absenteeism and higher retention via lower burnout rates keep the health system running smoothly.
Such benefits are worth hundreds of millions of dollars in Quebec. The financial upside justifies financial investment. Leaders with limited fiscal leeway are well served to recognize this.
Pharmacies and clinics are critical nodes for any health network seeking to maximize the impact of their patient redirection initiative. Dollars saved are redistributed throughout the health system, improving patient outcomes and provider wellbeing while stabilizing the system for years to come.
In summary: When pharmacies are treated as resources for patient redirection, economic benefits compound.
Use pharmacies to enable system-wide efficiency
The pharmacies in your network hold enormous potential.
The Petal Patient Hub is made to tap it. The Hub redirects patients to unlock network capacity and improve patient outcomes system wide.
Our independent report explains how Petal helps the Government of Quebec redirect 800+ patients daily to more appropriate care settings while generating $2M per week in economic benefits and achieving 12.5% fewer low-acuity ED visits (CTAS 4–5).
The Hub’s advanced features include:
- Centralized care requests to capture patient preferences and history in one place.
- Integration with EMRs, PMS, and online booking portals to match patients with available providers.
- Predicted demand to drive high impact resource allocation.
Let’s make more of your existing resources and better satisfy every stakeholder.
Reduce ED overcrowding for patients and providers: