Key takeaways
- Billing and scheduling are operationally interdependent: Treating them separately creates blind spots, while aligning them connects workforce decisions to real demand.
- Better alignment increases coverage without increasing headcount: Billing data supports smarter shift coverage, reducing overtime spikes and uneven workload distribution.
- Transparency builds trust and supports retention: When clinicians understand how decisions are made, fairness becomes accessible to all.
To maximize limited time and budgets, healthcare billing and scheduling must work collaboratively.
When financial strain meets limited staff capacity, clinicians and health network decision-makers struggle to maximize resources. Staff become fatigued, as reflected in 46% of Canada’s physicians reporting high levels of burnout. Administrative burden keeps rising with 49% of family doctors surveyed by the College of Family Physicians of Canada working beyond capacity.
But integrating your scheduling and billing tools drives immediate, measurable impacts across organizations. The performance boost unlocks capacity and guides sustainable growth. Better care delivery follows.
Here are five reasons to stop seeing billing and scheduling as separate challenges and instead solve them together within modern healthcare environments.
1) Improve morale and decrease absences with reliable, trusted schedules
A reliable schedule is a primary predictor of healthcare workforce morale.
When clinicians trust that their shifts are accurate and fair, they plan their personal lives with confidence. This sense of predictability reduces stress and directly impacts attendance. Unfortunately, many care providers find last-minute changes, unclear assignments, and perceived favoritism facilitating frustration that leads to disengagement and unplanned absences.
Integrating billing and scheduling helps eliminate many of these issues at the source.
For example: If an emergency department (ED) physician receives a schedule based on historical demand and physician preferences, they’re engaged. Conversely, if the schedule leaves them struggling to meet patient demand due to understaffed shifts, or if they notice the same colleagues consistently assigned fewer nights or lighter workloads, their frustration builds.
Transparency is also key to schedule fairness. Here’s why:
- When clinicians understand how schedules are created and how decisions are made, they’re less likely to question why schedule decisions are made.
- A unified system that connects scheduling logic with billing realities ensures that shifts are aligned with current workload and compensation structures.
Impact: Consistency builds a positive feedback loop. Reliable schedules improve morale, which reduces absenteeism, which improves operations, and smoother operations help more patients.
CHUM saves 8,000+ scheduling hours per year using Petal Workforce.
2) Increase coverage with your existing staff while reducing burnout
Healthcare organizations must balance adequate coverage and staff exhaustion.
Hiring more clinicians is rarely feasible given organizations’ limited budgets. The more practical approach is to optimize how existing staff are scheduled and utilized.
When billing and scheduling systems operate in silos, opportunities for efficiency are often missed. Schedules don’t reflect real patient demand, leading to overstaffing in some periods and gaps in others. But by aligning scheduling with billing data, organizations gain a clearer view of ideal resource management.
This enables more precise shift allocation without increasing total hours worked.
Coverage improves when billing is considered, supporting teams and patients. You’ll more effectively:
- Staff high-demand periods based on billed activity.
- Highlight service intensity to match clinicians with patient needs.
- Identify patterns in overtime and premium pay.
Impact: When scheduling considers billing activity, decisions are based on real activity instead of assumptions.
3) Strengthen retention through autonomy, fairness, and transparency
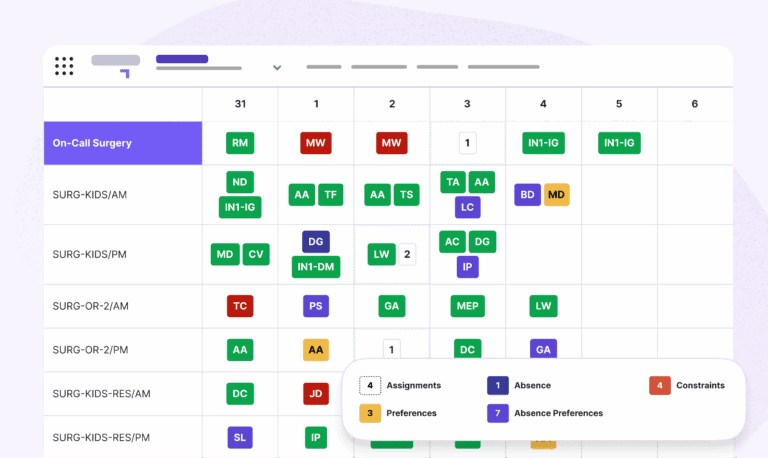
To retain healthcare professionals, they need—at least—a satisfactory work environment. Scheduling plays a central role in their experience.
When staff have control over their time and staff assignment processes, they feel satisfied. This has far-reaching benefits in any healthcare organization. Giving clinicians the ability to express preferences, swap shifts, or participate in schedule creation increases their sense of ownership. A modern approach to scheduling emphasizes autonomy.
Fairness is equally important.
Perceived inequities like uneven distribution of night shifts undermines team cohesion. Integrated scheduling systems apply consistent rules across the board. This ensures workloads are balanced, and that no physician is unreasonably burdened.
Transparency reinforces both autonomy and fairness. When clinicians see how schedules are generated and understand the factors influencing decisions, they’re more likely to accept outcomes, even when not ideal.
When billing data is part of this equation, transparency deepens. Clinicians better understand how scheduling decisions are shaped by workload, case complexity, and compensation structures. This reduces ambiguity around why certain shifts are assigned, so opportunities are distributed in a way that feels grounded in reality.
Impact: Connecting billing and scheduling helps organizations move from perceived fairness to demonstrable fairness.
Clinicians save 3.1 hours per week using Petal Billing.
4) Mobile-first change management empowers staff to own their time
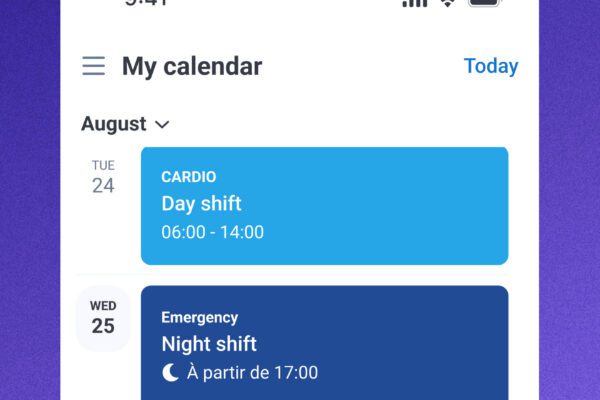
Mobile-first tools reshape how healthcare staff interact with scheduling systems.
Clinicians expect the same level of accessibility and ease of use in their professional tools as they do in their personal apps. Healthcare leaders need to meet this expectation to maintain high levels of staff satisfaction.
Mobile-first scheduling platforms—such as the Petal Health Mobile App (App Store / Play Store)—allow staff to access their schedules anytime, request changes, receive updates, and communicate in real time. In parallel, mobile access to billing tools gives clinicians visibility into their activity, workload, and captured revenue without requiring a switch to desktop.
Today, adoption is a major hurdle in implementing new systems. Mobile accessibility lowers this barrier by fitting naturally into existing workflows.
Here are four ways mobile access empowers staff:
- View and manage schedules in real time.
- Submit billing or activity data closer to the point of care, improving accuracy.
- Understand how shifts and compensation align across systems.
- Respond faster to changes.
Successful change management depends on aligning technology with user behavior. This contributes to job satisfaction while reducing administrative burden on managers, who shift their focus from coordination to strategic oversight.
Impact: When clinicians manage aspects of their schedule and billing responsibilities directly, they gain a stronger sense of control over their time and output.
5) Respect rest periods and overtime thresholds from the start
Compliance with labor regulations and industry standards should be fundamental in healthcare scheduling.
Rest periods and overtime thresholds are critical safeguards for staff and patient wellbeing. When scheduling is disconnected from billing and compliance systems, these rules are applied reactively. This leaves clinicians scheduled in ways that inadvertently violate rest requirements or trigger excessive overtime.
- In 2023–2024, 8% of hours worked by front‑line providers (excluding physicians) in hospital nursing units were overtime—22.6 million hours, equal to 11,500 full‑time positions.
An integrated approach allows these constraints to be embedded directly into the scheduling process. As shifts are created, the system automatically accounts for required rest periods, maximum hours, and overtime limits. Schedules are compliant from the outset, and the need for manual adjustments is reduced.
Proactive compliance also supports better financial management. Aligning scheduling decisions with billing data allows organizations to monitor and manage costs more effectively while still maintaining coverage.
For paramedics, respecting rest periods is especially important. The physical and mental demands of the role mean sufficiency recovery time is vital for reducing fatigue, improving performance, and lowering the risk of errors. When paramedics see their wellbeing prioritized in scheduling decisions, trust in the organization increases.
Impact: Building compliance into the foundation of scheduling creates a safer, more sustainable work environment.
Maximize your resources. Satisfy your team and patients.
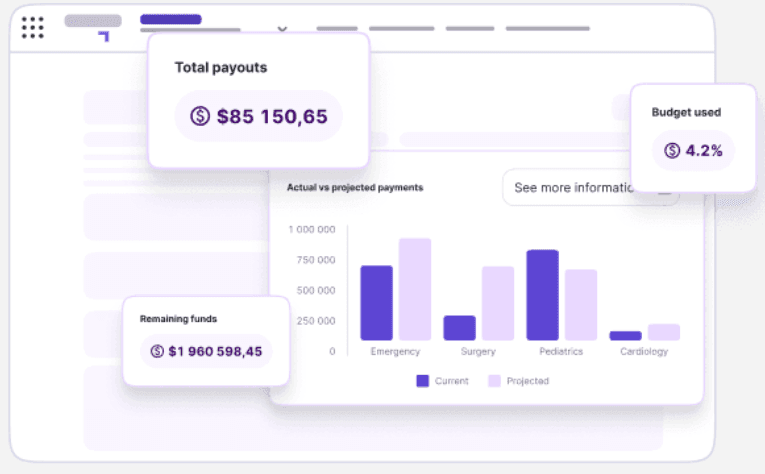
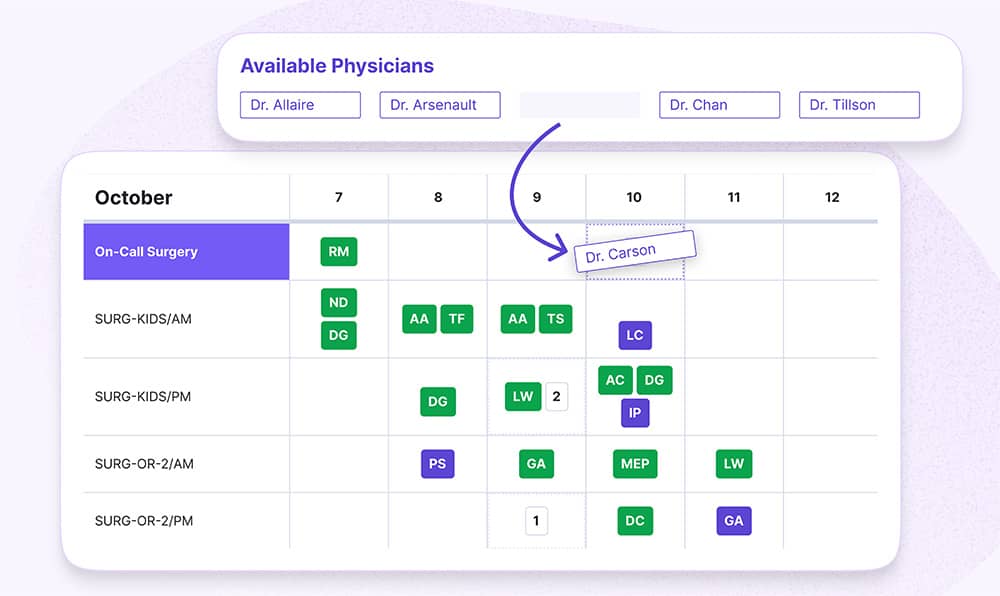
Combined billing and scheduling is within your reach.
Because Petal provides both.
Petal Workforce let’s you build optimized, automated schedules in minutes while reducing manual errors. Petal Billing simplifies billing processes using tools designed for unique billing rules across Canada.
- Proof: CHUM reduced scheduling time by 98% using Petal Workforce. Physicians using Petal Billing reported an annual average of 161 hours saved and 9.4% more revenue.
Your patients and providers gain when your operation thrives.
Make scheduling and billing work for you:







