Key takeaways
- Integrate workforce and billing to drive revenue growth through streamlined workflows and real-time visibility featuring all users on a single platform.
- Reduce administrative burden to improve staff morale, leading to faster patient care and improved care outcomes.
- Connected, consolidated tools reduce organizational silos to strengthen coordination by limiting operational bottlenecks.
Today’s healthcare organizations must do more with less.
Budget strain paired with provider shortages leaves clinicians, their teams, and health network decision-makers struggling to maximize resources. Clinics and hospitals struggle to meet patient demand. Staff become fatigued, as reflected in 46% of Canada’s physicians report high levels of burn out. Administrative burden continues to rise with 49% of family doctors surveyed by the College of Family Physicians of Canada working beyond their capacity.
Margins are tightening while expectations for access, quality, and experience grow.
Taking steps to combine workforce management (WFM) and billing tools prepares transformative impacts on healthcare providers and delivery organizations. When these tools operate in isolation, users in clinics, hospitals, and health networks face unnecessary friction. When they work together, teams unlock capacity to guide sustainable growth and better care delivery.
Read on to explore five key reasons why connected workforce and billing tools are invaluable in modern health systems.
1. Drive scalable growth without more effort
Growth in healthcare should mean serving more patients and expanding programs. Administrative complexity and disconnected systems too often get in the way and cause operational bottlenecks that limit scale. Distinct scheduling, billing, and reporting tools require manual reconciliation, which slows teams down.
- What’s efficient scaling? When providers develop their services and staffing models without proportionally increasing administrative overhead.
Scheduling decisions support service delivery and guide future reimbursement. When teams focus on expanding services rather than troubleshooting schedules, they unlock time for developing new care programs or optimizing existing ones. An advanced billing solution will then measure programs’ return on investment more efficiently than manual efforts.
Impact in action: Aligning workforce management with billing simplifies daily operations by removing system friction.
CHUM uses Petal WFM to reduce schedule creation time by 98%.
2. Use one vendor to cut costs and simplify operations
Saving money shouldn’t mean sacrificing staff wellbeing. Single vendor operations achieve both financial savings and improved care outcomes while simplifying day-to-day activities for care teams. Using a single technology provider for closely related workflows like workforce management and billing provides a strong financial rationale. Fewer vendors means lower integration costs and simplified support.
Then the benefits go beyond budgets. The intangibles include:
- Smoother, more intuitive workflows that decrease delays and miscommunication.
- More satisfied staff who feel less burnt-out.
- Less time wasted navigating fragmented systems.
When schedules, on-call coordination, and billing processes align, care teams have more energy for patients.
Impact in action: Patients notice when providers are coordinated and satisfied. Engagement supports more positive care experiences and better health outcomes.
3. Reduce administrative burden to save time for patients
Care team members only have 24 hours in their days too. This means maximizing that time is critical to public health success, so less administrative work and stronger care coordination are top priorities. Coordination breaks down when teams rely on fragmented systems. Information gets lost between hand-offs and miscommunication increases, leaving teams to spend valuable time fixing errors or duplicates.
When workforce management and billing tools connect, time is returned to patient care.
- For current billing users: Access to workforce scheduling information reduces manual entry and guesswork. Claims are supported by accurate, timely data.
- For current workforce users: Automated billing helps ensure that clinical activity leads to revenue growth. Financial sustainability is reached without extra effort.
Ultimately, patients benefit if their providers have time for them. When operational systems work to aid rather than hinder care coordination, patient interactions become a more prominent part of care provider schedules.
Here’s how connected workforce and billing tools break down organizational silos:
- Shared data creates a common basis for communication.
- Teams see how staffing decisions affect service delivery.
- Care outcomes improve, and results are efficiently captured by billing.
Impact in action: Reduced administrative burden allows clinicians to focus on consultations, follow-ups, finances, and more.
Clinicians increase revenue by an average of 9.4% using Petal Billing.
4. Gain greater visibility to make better decisions
Good decisions depend on good information. Disconnected systems make it harder to see the full picture—especially when workforce management and billing tools are misaligned. Pairing them gives group leaders clearer visibility into how staffing, service delivery, and financial outcomes guide better care.
- Key: A single, connected view allows leaders to easily compare workforce patterns with billing performance, as well as justify budgets when shadow billing is compulsory.
Simplified scheduling operations make life easier for both teams and patients, improving predictability and access. Instead of responding to problems after they surface, such as missed revenue, staffing shortages, or patient delays, leaders anticipate challenges. They adjust before problems escalate.
Impact in action: Integrated visibility enables proactive rather than reactive decision-making to benefit patients and providers.
Schedule smarter. Grow revenue. Petal is here for both.
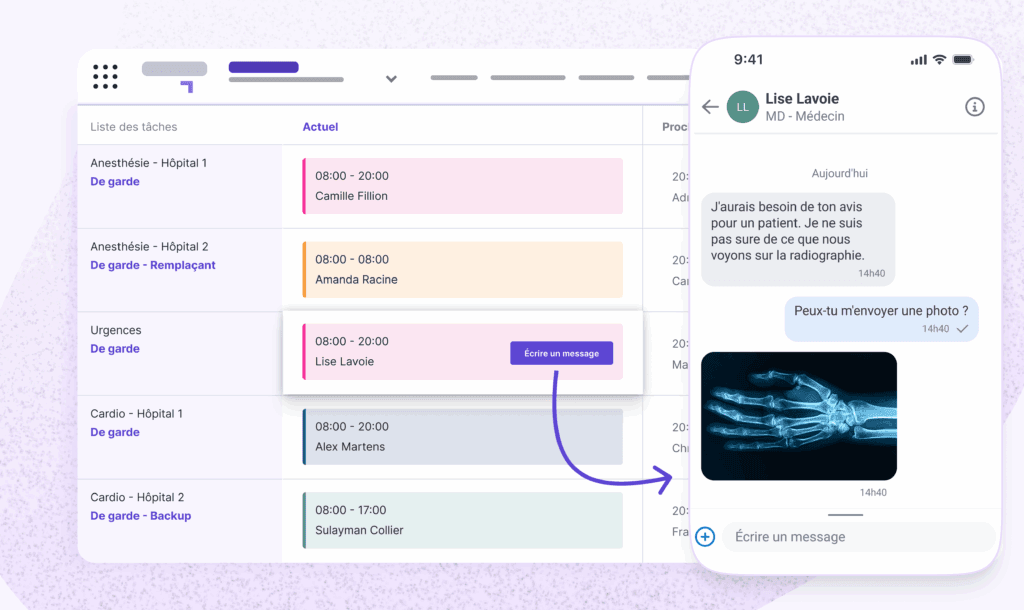
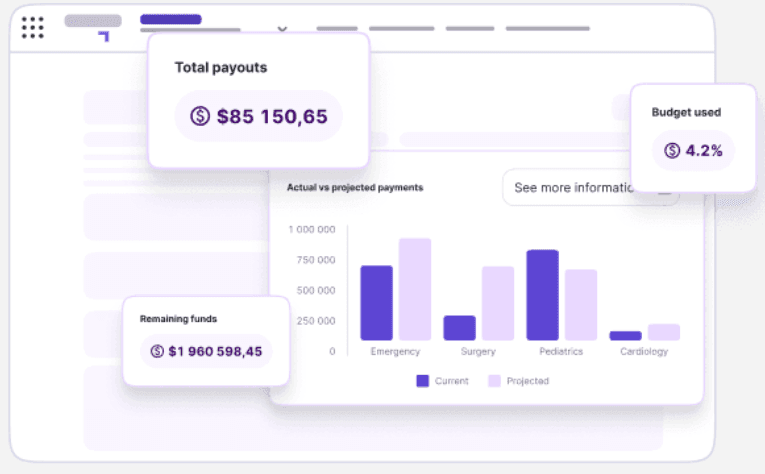
Your workforce management and billing work better together. We’re here to bridge the gap.
Petal Workforce and Petal Billing provide solutions to help teams across the care continuum unlock care capacity. Access the benefits:
Petal Workforce
Real-time dashboards of capacity by provider type and specialty;
Secure messaging between teams and departments;
Simplified on-call coordination with single source visibility;
Petal Health Mobile App for access anywhere.
Proof: CHUM used Petal Workforce to achieve 98% less time spent creating workforce schedules, 92% staff satisfaction among users, and a 70% reduction in scheduling costs by replacing manual tools.
Petal Billing
Provincial code validation and error checking;
Real-time claim status and remittance tracking;
Live billing agents to support any time;
Visibility across hospitals, programs, and care settings.
Proof: Physicians using Petal Billing reported an average revenue increase of 9.4% compared to manual billing. This equates to 161 hours saved annually at a value of $24,123 per year.
Petal combines automation, personalized support, and end-to-end claim management to eliminate the friction that slows clinics down. You’ll receive faster, more intuitive billing workflows to support short- and long-term success.
Gain confidence knowing every claim is complete, compliant, and optimized before submission. Talk to a Petal expert to get started today.







