Key takeaways
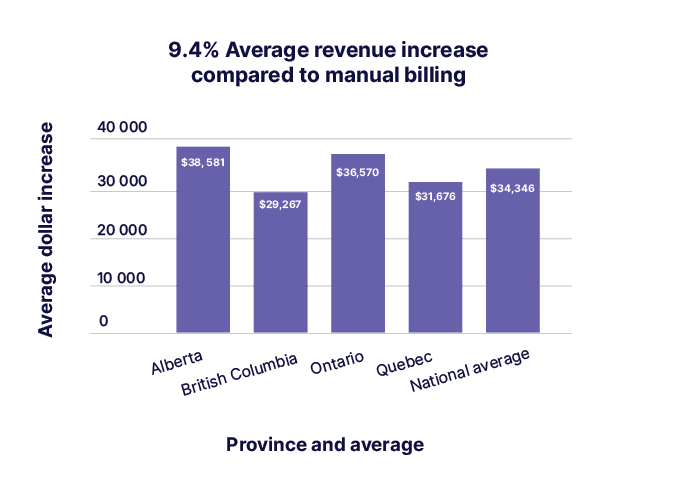
- Average revenue lift: Physicians reported a 9.4% increase in annual billings—about $34,346 nationally, with province‑level estimates of $38,581 (AB) and $31,676 (QC).
- Time savings with measurable value: 3.1 hours/week freed from admin, worth roughly $24,123/year based on national remuneration benchmarks.
- Net impact: Revenue optimization plus time value pushes annual ROI well above $50K per physician, depending on practice profile and province.
Billing: The lifeline—and the bottleneck—in fee‑for‑service care
In Canada’s fee‑for‑service (FFS) environment, billing drives physician income but often drags down productivity.
Complex, province‑specific rules, evolving codes, and preventable errors create friction that puts pressure on revenue and time. With most Canadian physicians affected by FFS (about 70% of payments nationally; ~96% of doctors impacted), optimizing billing isn’t a nice‑to‑have, it’s a revenue strategy.
A new independent study—led by a health economist—quantifies that strategy: modern billing solutions materially increase revenue while freeing measurable time.
The revenue story: A consistent 9.4% lift
Across respondents, physicians estimated an average 9.4% increase in annual billings after adopting a medical billing solution. Applied to benchmarks, that equates to $34,346 nationally, $38,581 in Alberta, and $31,676 in Quebec. The mechanism is straightforward: more complete claims, fewer errors, and better use of available modifiers.
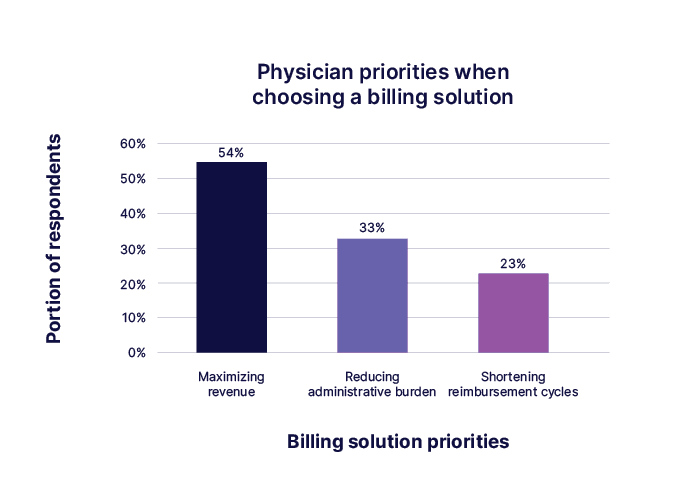
Those gains align with user priorities. When asked what matters most in a billing platform, “maximizing revenue” ranked #1 (54%), ahead of administrative relief and reimbursement speed. This is clear evidence that physicians seek tools that systematically capture income they’ve already earned. This is only one part of the value side of the impact billing solutions have for physicians.
Time is money: 161 hours a year back
Revenue growth is only half the ROI picture. The study also found 3.1 hours/week, or 161 hours per year, of administrative time saved compared to manual billing. That’s a 24% reduction in admin workload when mapped to national time‑use data. Valued at the average hourly rate derived from national clinical payments, that’s $464/week or $24,123/year.
Whether that time goes to patient care, teaching, research, or simply reducing burnout pressure, its value compounds. This is especially true in busy practices where small process improvements translate into steadier cash‑flow and fewer after‑hours catch‑up sessions.
Where the gains come from (and why they persist)
Physicians rated optimization of billing codes and modifiers as the most valuable feature—87% called it “extremely valuable”—followed by real‑time error validation and staying current with provincial billing rules and fee codes. Together, these capabilities reduce missed claims, fix errors before submission, and capture complex, legitimate opportunities that often slip through manual workflows.
Platform performance data supports the outcome side of the equation: among thousands of annual claims per user, final denial rates were just 0.8% after correction and resubmission, indicating that automation plus expert review gets claims paid. This is significant when you consider that up to 8% of manual claims are rejected.
CHUM reduced scheduling time by 98% using Petal Workforce Management.
Why ROI matters right now
With FFS still dominant, small inefficiencies scale quickly: a few missed modifiers or recurring rejections across hundreds of claims amount to tens of thousands of dollars of foregone income. In many cases, clinicians and health delivery organizations do not even follow up on rejected claims due to internal administrative burden.
Our healthcare system remains in a climate of rising workload and persistent administrative pressures, and having billing efficiency is the fastest, lowest‑disruption lever for practice‑level financial performance.
Apply the numbers to your practice
Use the study’s benchmarks to estimate your potential upside:
- Start with your last 12 months of billings and apply the 9.4% revenue lift to get a directional figure.
- Add the time value (3.1 hours/week × your effective hourly rate) to see the efficiency dividend.
- Scan your workflow for error‑prone steps—modifier selection, complex codes, and real‑time validation are the highest‑value fixes.
Example: A physician at Canada’s average remuneration adds approximately $34K in revenue and $24K in time value annually by moving from manual to modern billing. This rolls up to a combined impact well over $50K.
Choosing an approach that fits (self‑entry vs. supported)
Ready to quantify your ROI?
Download the full billing report for province‑specific benchmarks and the methodology behind the findings. Then map the numbers to your workload and claim mix to forecast your practice‑level impact.
Grow revenue while making more time for patients:







